Homebound Criteria
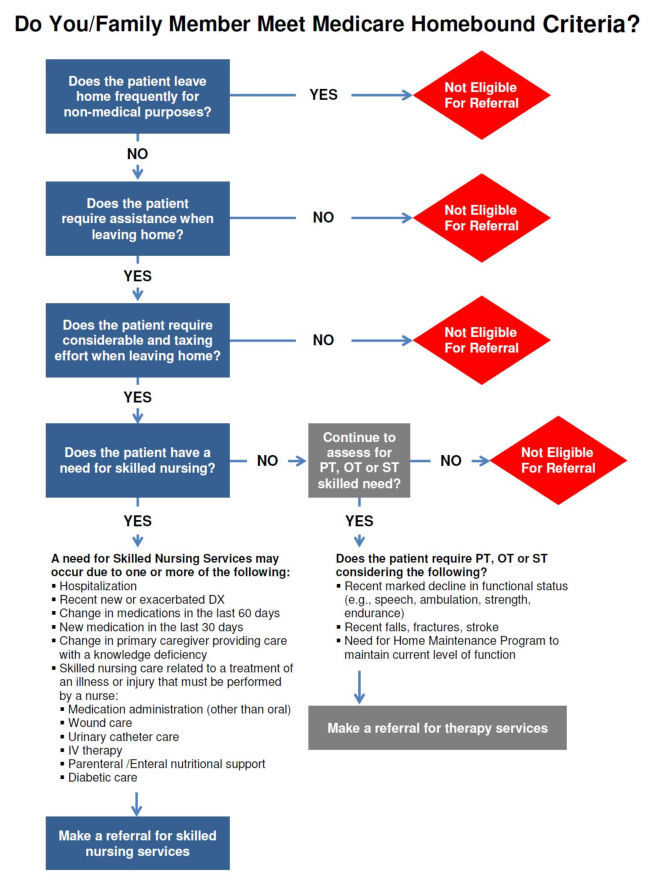
Medicare Home Health Homebound Criteria
Medicare defines an individual as homebound if he/she:
- Is unable to leave the home due to an illness or injury (not just due to weakness and feebleness or old age)
- Experiences a considerable and taxing effort to leave and is absent from the home infrequently, for a short duration, or to receive medical care
- Requires the assistance of a device, other persons or special transportation
Homebound eligibility is not affected by frequent absences from the home when the reason for leaving is to receive medical care, provided the home health services could not reasonably be provided by the other medical care providers.
CMS was asked by Congress to refine the definition of Homebound status, and added the following
information:
- The new definition explicitly allows absences from home to participate “in therapeutic, psychosocial or medical treatment in an adult-day-care program that is licensed or certified by a state.” Such absences will not be considered violations of the homebound criteria.
- Additional clarification includes that absences to attend religious services will be considered an “absence of infrequent or short duration,” and allowable under the homebound definition.
An individual would NOT be considered homebound if he/she:
- Leaves the home frequently for social activities
- Goes to a daycare center for non-medical purposes or to a relative’s house part of the time (except
Alzheimer’s-specific daycare centers) - Leaves the home against physician’s orders, if this is done frequently or for long periods of time
- Leaves the home for shopping or business on a regular basis
Home Health Provides:
- Medicare Home Health Homebound Criteria
- Observation & Assessment of Condition
- Patient & Family
- Education of Disease Process
- Management & Evaluation of Patient
- Care Plan
- Medication Education & Management
- Dressing Changes
- Home Safety & Emergency Education
- Gastrostomy Care
- Wound Care
- Tracheostomy Care
- Catheter Care
- Enteral & Parenteral Nutrition
- Injections
- Venipuncture
- IV Therapy
- Ostomy Care
- Pain Management
- Diabetic Care
- Nutritional Support
- Anodyne® Therapy
Medicare will pay for home care visits when the following criteria have been met:
The patient must be enrolled in the Medicare program during the time the services are provided and be eligible for benefits.
A Medicare-certified agency must provide services.
- A physician who establishes and periodically reviews the plan of care at least every 60 days must order the services.
- Services must be provided in the patient’s place of residence.
- The patient must be homebound.
- The services must be medically reasonable and necessary to the treatment of an illness or injury.
- The patient must need a qualifying skilled service (Skilled Nursing, Physical Therapy, Speech Therapy on an intermittent basis or continued care from an Occupational Therapist.)
If at least one of the qualifying services is needed, Medicare covers the following services: home health aide services, medical social services, medical supplies, and durable medical equipment and supplies.


